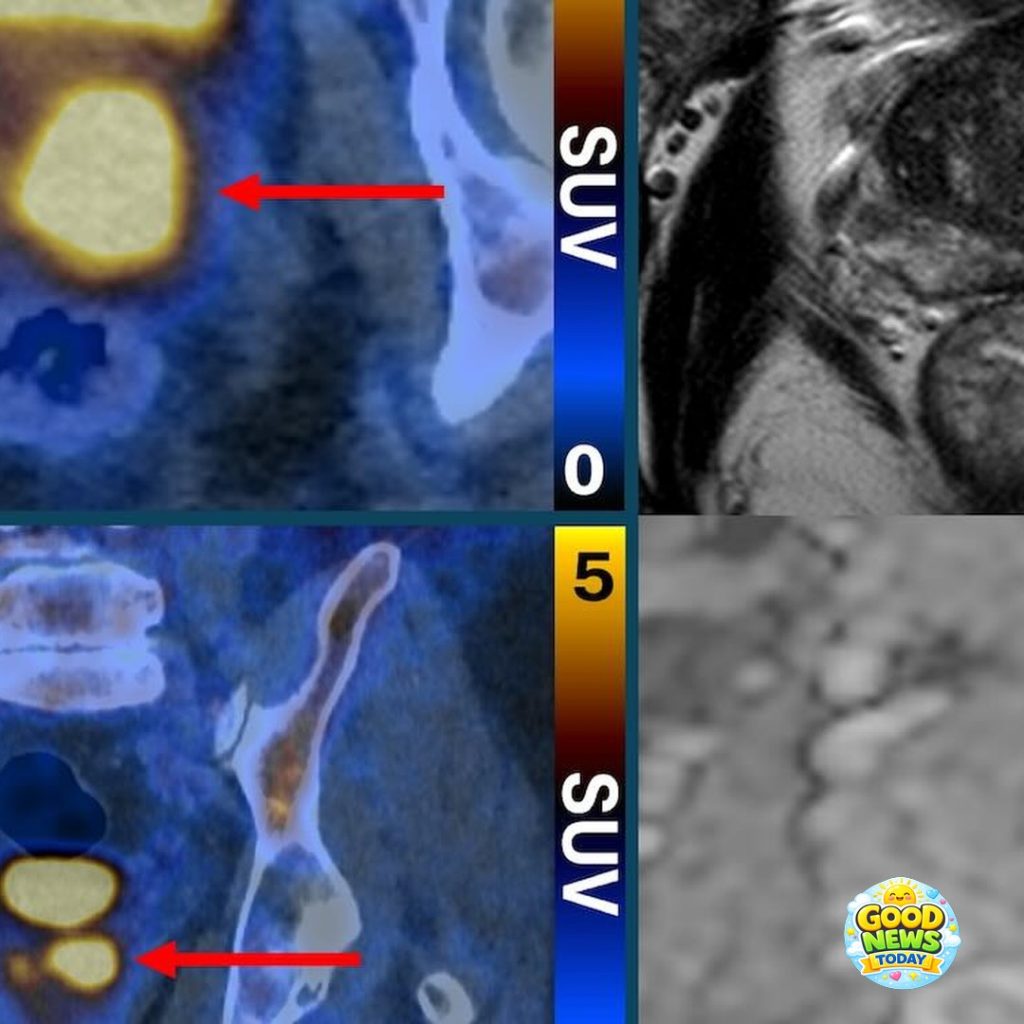
Exciting advancements in prostate cancer detection are making a significant impact on patient care by employing innovative scans that illuminate cancer cells. These remarkable imaging tests, already accessible in Australia and Europe, have the potential to eliminate the necessity for invasive biopsies.
Using a specialized molecule that attaches to prostate cancer cells, this advanced imaging technique causes the cells to “glow,” presenting bright spots on the scan images. Australian scientists assert that this groundbreaking method could safely reduce the number of men requiring a biopsy by half after inconclusive MRI results.
The PSMA PET/CT scan is adept at identifying more aggressive prostate cancer cells, which could pose a threat and require treatment. Additionally, it plays a crucial role in minimizing over-diagnosis by differentiating between low-risk cancers that are unlikely to cause harm and those that need attention.
Dr. James Buteau, a nuclear medicine physician at the Peter MacCallum Cancer Centre in Melbourne, expressed enthusiasm about the power of this imaging technique, stating, “It’s rare to see such strong imaging that could be so powerful in the clinic.”
Prostate cancer is a leading cause of cancer-related deaths among men, with approximately 1 in 8 men receiving a diagnosis. Typically, these individuals undergo MRI scans to detect any abnormal growths. When MRI results are suspicious or unclear, the standard course of action is a biopsy, which involves extracting small tissue samples from the prostate. However, this invasive procedure can be uncomfortable and carries potential side effects, leading to anxiety for many patients.
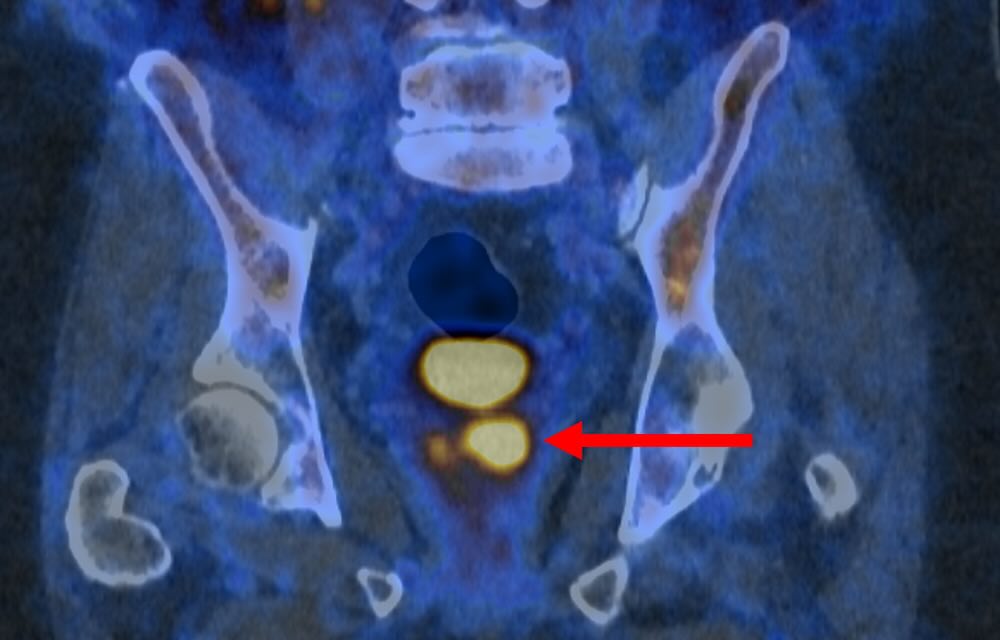
Implementing this new testing method into clinical practice could significantly address the critical issue of over-diagnosis in prostate cancer. This situation can lead to unnecessary and sometimes detrimental treatments for cancers that would not have caused harm.
The Primary2 trial, which focused on men at higher risk for prostate cancer—such as those with a strong family history—randomly assigned participants to either receive a standard biopsy or the PSMA PET/CT scan. The findings revealed that the PSMA PET/CT scan could accurately identify individuals who did not have cancer or whose cancer was so low-risk or slow-growing that it would likely remain harmless.
As a result, many patients were spared the need for a biopsy, while those with positive cancer results from the PSMA PET/CT scan proceeded with the procedure. Remarkably, this approach halved the number of biopsies performed without missing any cases of harmful cancer.
For those who still required a biopsy, the scan results enabled targeted procedures to focus on the suspicious areas identified, thereby reducing complications and enhancing accuracy.
The outcomes from the Primary2 trial mark an exciting milestone, as researchers will continue to follow the 660 participating patients for two years to gather further insights.
With the PSMA PET/CT scan already making waves in Australia, this innovative approach represents a promising leap forward in the fight against prostate cancer.